PLEASE go to this website and take the Stillbirth survey located on the upper right hand of the page. This is a beginning for research we are proposing.
www.aplacetoremember.com
Thursday, May 20, 2010
Friday, May 14, 2010
24 week ultrasound visit
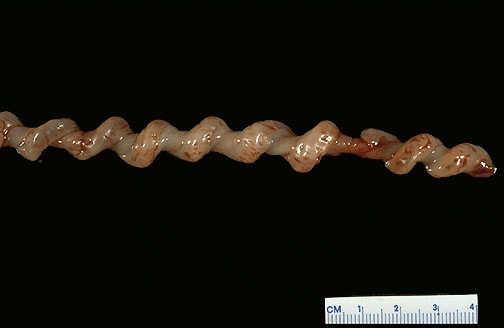
I was told yesterday, while receiving an ultrasound from my high risk doctor's office, that the techs have jsut been instructed that if they see a true knot in the umbilical cord while scanning, they are not to tell the patient. It doesn't cause any concern, babies are born all the time with them. No need to worry the patient. So just don't say anything. In the tech's humble opinion, she consoled me ( I was angry about this), what can be done anyway? Babies are either going to live or not. There is very little the OB community can do. Again, that was her opinion.
And she was directed by the best of the best here in AZ.
I'm upset. I am most upset that doctors would get together, make a statement and policy and set it in force without any research to back up their theory. Yes, babys are born fine with knots present. Then again, babys are also born dead like that. Babys are born fine with cord torsion. Then again, some are born dead, and others suffer medical problems all their life, such as autism and cerebral palsy.
When a doctor tells me that the cord is fine, normal, when twisted or knoted, etc. I say, "Yes, the cord is fine. Until it's not. The baby is fine. Until that moment when there is blood constriction and he's dead."
I am under-educated, not medically qualified, and I feel helpless. I see the resistance from educated, qualified people to be open to new information or research about prenatal care. I wonder why... and in this I see human limitations and personality quirks. We are all resistant to change, aren't we?
At 22 weeks I told my doctor I am concerned about my low blood pressure because there is scant research linking it to stillbirths. She instantly dismissed it and said that she's sure the mother who loses her baby at night must also have genetic factors involoved, be laying on her back, or have some other complication that coincides with low blood pressure. Basically, I have never seen this study, so it's probably not true. There are other possible explanations so I am going to go with those.
I was, surprise, not satisfied! I said, "Unfortunately, there isn't research on this happening, so we have no way of knowing whether low blood pressure is or isn't a factor. Isn't is safer as a scientist to not assume it's wrong but instead wait for it to be disproved before you dismiss it?"
She smiled and sent me on my way, probably happy the annoying, paranoid mother was gone.
For thoughtful consideration, here is a small paragraph from one report published this year concerning the need to change prenatal care in regards to acknowleding that cord accidents may be measureable and preventable.
I especially like the end, which states that one COMMON prenatal practice has absolutely no standing, yet is commonly used.
(Emphasis added by myself)
Hypoactivity, decreased fetal movement, should be investigated with the objective to rule out umbilical cord entanglement and UCA especially in no risk patients with previous normal activity.[599-602] Decreased fetal movement that is sustained in early pregnancy (20wks-28wks) may indicate several fetal conditions. IUGR, Genetic Skeletal Muscle Disorder, Congenital Anomalies and or a fetal condition that “weakens the fetus”. Studies investigating fetal movement counting have been unable to show a definitive influence on outcomes.[599] The benefit of observing the fetus begins with the 18wk-20wk onset of movement detection by the mother. Fetuses change their movement pattern over time and become repetitive by 26wks-28wks. The initial investigation of fetal behavior should include questioning the mother at her prenatal visit about this detectable pattern. Studies have failed to look at the spectrum of fetal behavior and focused on one behavior of no fetal movement. No fetal movement is an alarm from the fetus to investigate the pregnancy immediately. Patients should be sent to the nearest obstetrical clinic or labor&delivery unit for evaluation. There are no studies to support recommending to a mother to put her feet up or drink fluids when there is a complaint of no fetal movement. Glucose ingestion and meals does not alter fetal behavior.[595],[603],[604],[605] The defining study on fetal behavior observation and outcomes in first time moms and previous stillbirth moms has not as yet been done. [143],[606],[607],[608],[609],[610],[611].
And she was directed by the best of the best here in AZ.
I'm upset. I am most upset that doctors would get together, make a statement and policy and set it in force without any research to back up their theory. Yes, babys are born fine with knots present. Then again, babys are also born dead like that. Babys are born fine with cord torsion. Then again, some are born dead, and others suffer medical problems all their life, such as autism and cerebral palsy.
When a doctor tells me that the cord is fine, normal, when twisted or knoted, etc. I say, "Yes, the cord is fine. Until it's not. The baby is fine. Until that moment when there is blood constriction and he's dead."
I am under-educated, not medically qualified, and I feel helpless. I see the resistance from educated, qualified people to be open to new information or research about prenatal care. I wonder why... and in this I see human limitations and personality quirks. We are all resistant to change, aren't we?
At 22 weeks I told my doctor I am concerned about my low blood pressure because there is scant research linking it to stillbirths. She instantly dismissed it and said that she's sure the mother who loses her baby at night must also have genetic factors involoved, be laying on her back, or have some other complication that coincides with low blood pressure. Basically, I have never seen this study, so it's probably not true. There are other possible explanations so I am going to go with those.
I was, surprise, not satisfied! I said, "Unfortunately, there isn't research on this happening, so we have no way of knowing whether low blood pressure is or isn't a factor. Isn't is safer as a scientist to not assume it's wrong but instead wait for it to be disproved before you dismiss it?"
She smiled and sent me on my way, probably happy the annoying, paranoid mother was gone.
For thoughtful consideration, here is a small paragraph from one report published this year concerning the need to change prenatal care in regards to acknowleding that cord accidents may be measureable and preventable.
I especially like the end, which states that one COMMON prenatal practice has absolutely no standing, yet is commonly used.
(Emphasis added by myself)
Hypoactivity, decreased fetal movement, should be investigated with the objective to rule out umbilical cord entanglement and UCA especially in no risk patients with previous normal activity.[599-602] Decreased fetal movement that is sustained in early pregnancy (20wks-28wks) may indicate several fetal conditions. IUGR, Genetic Skeletal Muscle Disorder, Congenital Anomalies and or a fetal condition that “weakens the fetus”. Studies investigating fetal movement counting have been unable to show a definitive influence on outcomes.[599] The benefit of observing the fetus begins with the 18wk-20wk onset of movement detection by the mother. Fetuses change their movement pattern over time and become repetitive by 26wks-28wks. The initial investigation of fetal behavior should include questioning the mother at her prenatal visit about this detectable pattern. Studies have failed to look at the spectrum of fetal behavior and focused on one behavior of no fetal movement. No fetal movement is an alarm from the fetus to investigate the pregnancy immediately. Patients should be sent to the nearest obstetrical clinic or labor&delivery unit for evaluation. There are no studies to support recommending to a mother to put her feet up or drink fluids when there is a complaint of no fetal movement. Glucose ingestion and meals does not alter fetal behavior.[595],[603],[604],[605] The defining study on fetal behavior observation and outcomes in first time moms and previous stillbirth moms has not as yet been done. [143],[606],[607],[608],[609],[610],[611].
See www.preginst.com, Prenatal Umbilical Cord Project 2010, page 20
Wednesday, February 10, 2010
Personal History
My name is Blue Haught. I am the father of two living children. My 3rd child was a full-term stillborn who died as the result of umbilical cord torsion (twisting & kinking). My 4th child was born at 30 weeks and survived only a few hours due to complications of fetal hydrops. My desire is to prevent unnecessary fetal deaths deaths and to seek answers as to why our previous two babies had to die. In addition, I am trying to understand if there are correlations with the two deaths. My wife and I have spoken with many doctors that were involved in the care of our two babies who died and they all were adamant that there was nothing that could have been done and that the deaths aren't related. New information has suggested to us that there absolutely was something that could have been done to possibly save our 3rd child and that there may, in fact, be a correlation between him and our 4th child's death. For a more detailed history on our family's plight click on the following link:
http://www.kellyandblue.blogspot.com/
I believe that if there was a database that allowed obstetricians to view data regarding numerous prenatal, maternal, and umbilical cord statistics of babies who die before and during birth, there would be enough information to make necessary changes in how pregnant mothers are monitored and thus provide beter opportunities to intervene when problems arise in utero. What I am proposing is that states or our national government make it manditory for hospitals to conduct a standardized, post-mortem survey of all fetal demises. The survey would include maternal history, obstetric history, exposre to dieseases, pesticides, and several other potential risk factors. Obviously the mother would have the right to refuse the survey, but the information that would be gleaned from such an inquiry would yeild much needed statistics that currently aren't available.
For a better, more medically-based rationale for this please visit the website of a pioneering physician in Louisiana who has researched this issue and found staggering results:
http://www.preginst.com/
Please have patience as I attempt to make this blog more public and userfriendly. I believe that one day, this database will be crediting with saving hundreds, perhaps thousands of lives every year!
http://www.kellyandblue.blogspot.com/
I believe that if there was a database that allowed obstetricians to view data regarding numerous prenatal, maternal, and umbilical cord statistics of babies who die before and during birth, there would be enough information to make necessary changes in how pregnant mothers are monitored and thus provide beter opportunities to intervene when problems arise in utero. What I am proposing is that states or our national government make it manditory for hospitals to conduct a standardized, post-mortem survey of all fetal demises. The survey would include maternal history, obstetric history, exposre to dieseases, pesticides, and several other potential risk factors. Obviously the mother would have the right to refuse the survey, but the information that would be gleaned from such an inquiry would yeild much needed statistics that currently aren't available.
For a better, more medically-based rationale for this please visit the website of a pioneering physician in Louisiana who has researched this issue and found staggering results:
http://www.preginst.com/
Please have patience as I attempt to make this blog more public and userfriendly. I believe that one day, this database will be crediting with saving hundreds, perhaps thousands of lives every year!
Subscribe to:
Posts (Atom)